Cardiovascular Gender Medicine

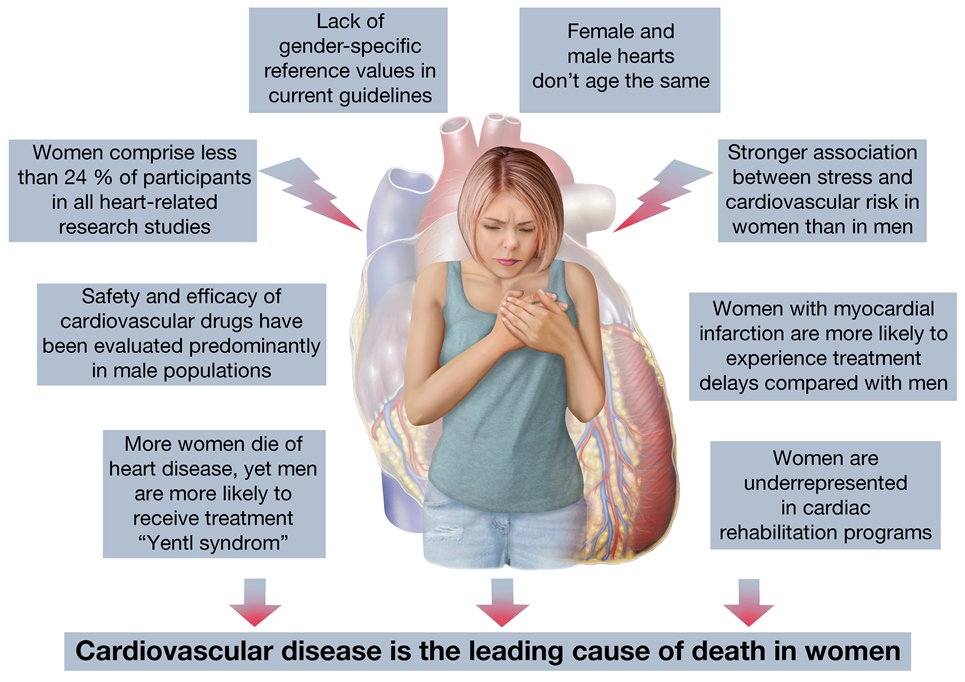
While cardiovascular mortality rates in men have steadily declined since the 1980s, the disease is becoming more common in women, with cardiovascular deaths in women currently exceeding those in men. In fact, clinical outcomes from acute coronary syndrome and heart failure are consistently worse for women than men (Figure 1). However, the gender-specific environmental, molecular, and cellular variables that contribute to cardiovascular disease are largely unknown; patients are treated the same regardless of sex.
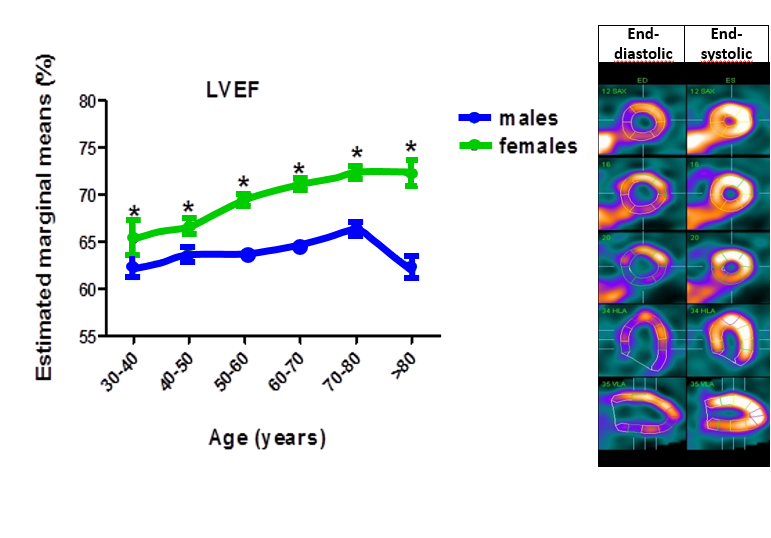
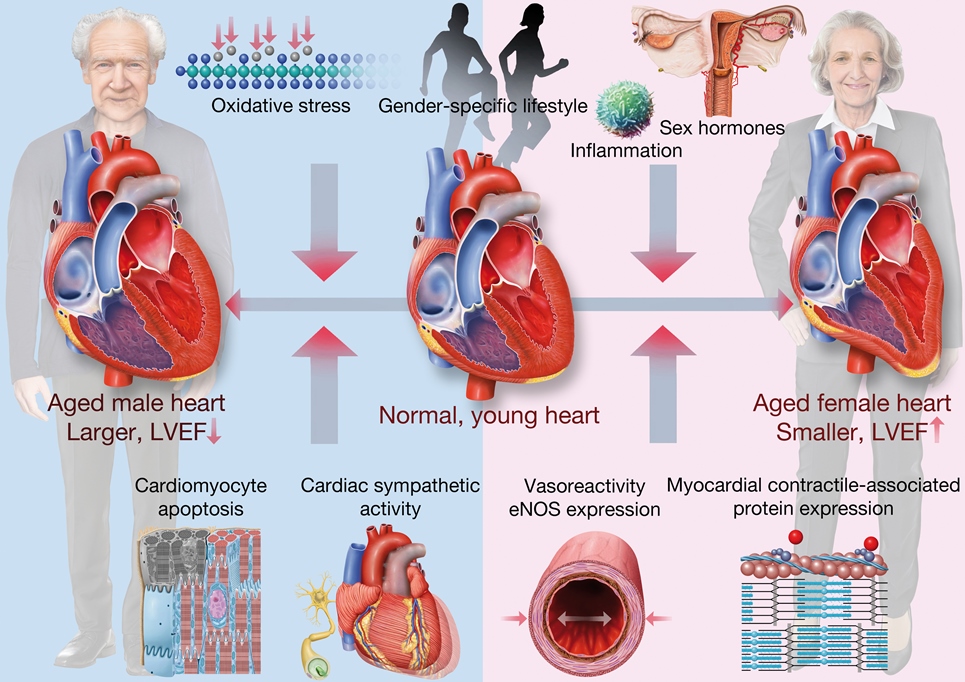
We recently observed significant sex- and age-specific differences in baseline left ventricular ejection fraction (LVEF), with a strong age-dependent increase in LVEF observed in healthy women but not in men (Figure 2). Given the prognostic importance of LVEF and its routine use in clinical decision making, understanding the variables that modulate myocardial contractility and vulnerability to cardiac injury in postmenopausal females and older males is of paramount importance for the development of personalized age- and gender-based therapies. In our current projects we therefore assess the impact of (patho)physiological factors contributing to sex- and age-related differences in cardiac function (Figure 3). More precisely, we are studying the extent to which these sex-differences can be attributed to sex hormones and their receptors, to differences in genetic predisposition, neurohumoral signalling, and gender-based lifestyle factors. For this purpose, we are using murine experimental models and a variety of in vivo imaging modalities including serial positron-emissions tomography, echocardiography and cardiovascular magnetic resonance imaging. Our ultimate goal is to improve and personalise gender-based therapeutic approaches in the aging population.
Key publications
- Gebhard C, Buechel RR, Stähli BE, Gransar H, Achenbach S, Berman DS, Budoff MJ, Callister TQ, Chow B, Dunning A, Al-Mallah MH, Cademartiri F, Chinnaiyan K, Rubinshtein R, Marques H, DeLago A, Villines TC, Hadamitzky M, Hausleiter J, Shaw LJ, Cury RC, Feuchtner G, Kim YJ, Maffei E, Raff G, Pontone G, Andreini D, Chang HJ, Leipsic J, Min JK, Kaufmann PA. Impact of age and sex on left ventricular function determined by coronary computed tomographic angiography: results from the prospective multicentre CONFIRM study. Eur Heart J Cardiovasc Imaging. 2016 Jul 26. pii: jew142.
- Gebhard C, Stähli BE, Gebhard CE, Fiechter M, Fuchs TA, Stehli J, Klaeser B, Tanner FC, Gaemperli O, Kaufmann PA. Gender- and age-related differences in rest and post-stress left ventricular cardiac function determined by gated SPECT. Int J Cardiovasc Imaging. 2014 Aug;30(6):1191-9.
- Gebhard C, Stähli BE, Gebhard CE, Tasnady H, Zihler D, Wischnewsky MB, Jenni R, Tanner FC. Age- and gender-dependent left ventricular remodeling. Echocardiography. 2013 Nov;30(10):1143-50.
- Fiechter M, Fuchs TA, Gebhard C, Stehli J, Klaeser B, Stähli BE, Manka R, Manes C, Tanner FC, Gaemperli O, Kaufmann PA. Age-related normal structural and functional ventricular values in cardiac function assessed by magnetic resonance. BMC Med Imaging. 2013 Feb 7;13:6
Home - Gebhardlab